MSSNY eNews: July 23, 2021 – It’s Time to Recharge Our Batteries
.Title
It’s Time to Recharge Our Batteries
Colleagues:
As I write this, I am on a long-awaited beach vacation with my family. My message to you this week is simple: after the long year-and-a-half we have all endured, it is time for us to step away and recharge our batteries. As physicians, we need to remember to take care of ourselves—so we are fully available for the care and well-being of our patients, families, and colleagues.
Taking a vacation is one way of stepping away and giving ourselves the opportunity to reset. But there are also many small things you can do to boost your personal well-being, including ensuring adequate nutrition, sleep, and exercise. Take a walk in the sunshine. Reconnect with a colleague. Hug your family.
The American Medical Association’s STEPS Forward program looks at the impact of well-being at both the individual and system level and offers strategies to promote individual well-being and resilience through the following steps:
- Get Organized
- Think About Your Physical State
- Think About Your Mental State
- Connect Socially
- Find Meaning In and Outside of Work
- Embrace Joy
- Reflect and Refine
For more information and to get started on your road to wellness, visit the AMA’s STEPS Forward website.
With the recent rise in the spread of the Delta variant in all 50 states, we still must protect ourselves, our families, and our friends by following the CDC’s COVID-19 guidelines.
Many of us missed taking time off last year. We are now able to travel and visit with family, friends, and those who have supported us in our careers. Enjoy, be well, and be safe!
Joseph Sellers, MD, FAAP, FACP
MSSNY President.
MSSNY Comments on Open Notes Rule in MedPageToday: “We Have to Be Careful About Unintended Consequences”
MSSNY President Dr. Joseph Sellers spoke to MedPageToday about Open Notes, the federal rule that requires clinical information like physicians’ notes and lab and imaging results to be made immediately available to patients.
“Communication of information is essential for our profession and our patients,” Joseph Sellers, MD, president of the Medical Society of the State of New York, told MedPage Today. “Having ways to get information to patients as effectively and timely as possible is great, but we have to be careful about unintended consequences.”
The criticism Sellers has heard from his medical colleagues centers around instances where patients get health information before physicians are able to help interpret it.
For instance, patients may receive pathology or imaging results electronically, prior to when their doctor is able to communicate with them via a phone call or office appointment.
A patient may find out bad news, and it may have been better for them to hear it first from their doctor, Sellers said. There may also be instances in which the complexity of test results makes them sound alarming, when they’re not. Or there are times when physicians can help break down details that are difficult for the average patient to understand and digest.
“I think that having that relationship between the physician and the patient is so important. It provides reassurance, it provides confidence to patients in the healthcare system,” Sellers said.
Read the MedPageToday article in its entirety here.
Clear Masks Improve Patient-Physician Communication
Effective patient-physician communication is crucial for developing trust, explaining complex concepts, and engaging patients in shared decision-making while also recognizing concerns and expectations. A key component to communication, though, is nonverbal communication—such as facial expressions—which has been disrupted during the COVID-19 pandemic by mask wearing.
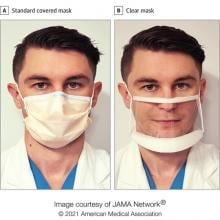
A study published in JAMA Surgery points to the effectiveness of clear masks as a way to overcome this perceived barrier to effective communication. When surgeons wore clear masks rather than the standard covered masks, patients rated their surgeon significantly higher in providing understandable explanations, demonstrating empathy, and eliciting trust.
Fifteen surgeons from a single academic institution were recruited by email. Before each clinic day, surgeons were randomized to wearing a clear or standard mask for each of their new patients, donning each mask type about half the time.
Last fall, 200 patients took part in this study. Each patient took a scripted, 10-question survey adapted from the Clinician and Group Consumer Assessment of Healthcare Providers and Systems survey. Other questions were added to assess surgeon empathy and trust, as well as a rating on the physician’s mask.
“Wearing clear versus covered masks suggests that not seeing the surgeon’s face negatively affects patient understanding, perceived empathy and trust,” says the study. “These findings should alert surgeons, because patient perceptions may not be detectable without purposeful attention to communication. We must make every effort to protect the sacred physician-patient relationship during these unprecedented times.”
Enhanced Communication and Trust
Overall, 93% of patients answered positively to the survey questions on communication, empathy, and trust. For the standard mask group, several questions were answered positively about 70% to 80% of the time. But for all questions, the clear-mask group answered positively at the same or greater frequency than the standard mask group.
The clear-mask group also had significantly more positive responses when answering two questions: Did the surgeon explain things in a way that was easy to understand, and did he or she seem to know the important information about the patient’s medical history?
On the explanation question, 95% of patients with surgeons wearing a clear mask said the doctor was easy to understand, compared with 78% of the patients whose surgeon donned a standard mask. Regarding the surgeon’s knowledge, 100% of patients in the clear-mask group responded positively, compared with 78% in the standard mask group.
Additionally, 99% of patients in the clear-mask group reacted positively about a surgeon’s empathy, compared with 85% in the covered mask group. Similarly, says the study, 94% of patients in the clear-mask group more frequently reported trusting their surgeon’s decisions, compared with 72% for the standard mask patient group.
Patient Excitement for Clear Masks
When asked about their impressions of the type of mask, 100% of the patients whose surgeon wore a clear mask had positive ratings. For standard masks, 72% of patients responded positively.
Patients were also asked to provide comments about their surgeon’s mask. Their opinions about clear masks were 93% were positive with one saying, “The clear mask was great. You should keep using it.” Only 5% of responses about the standard mask were positive, with many patients stating that they “don’t like masks” or that they were “sick of these masks.”
Mixed Results from Surgeons
Surgeons were also asked about their preference for mask type, with only 47% responding favorably to wearing clear masks compared to wearing standard masks during patient encounters. One-quarter of the surgeons said they would wear a clear mask if their patients preferred it.
However, many of the surgeons who took part in the study noted their own discomfort with the clear masks. They didn’t seem to fit as well, and they would fog up. Several surgeons also voiced concerns about the perceived level of protection provided by a clear mask even though the protection rating is equivalent to that of standard covered masks.
–Sara Berg, American Medical Association
Why I Am a MSSNY Member
KFF Report Finds Some Who Were Hesitant to Get a Vaccine in January Say They Changed Their Mind Because of Family, Friends and Their Personal Doctors
A new KFF COVID-19 Vaccine Monitor report finds that people who were initially hesitant to get a vaccine in January but ultimately did so often say that family, friends and their personal doctors helped change their minds.
The report features a second round of interviews with a nationally representative sample of adults six months after they first shared their vaccine intentions in January, early in the nation’s vaccine distribution effort. The new survey assesses whether or not they got a COVID-19 vaccine, the reasons behind their choice, and how they feel about their decision.
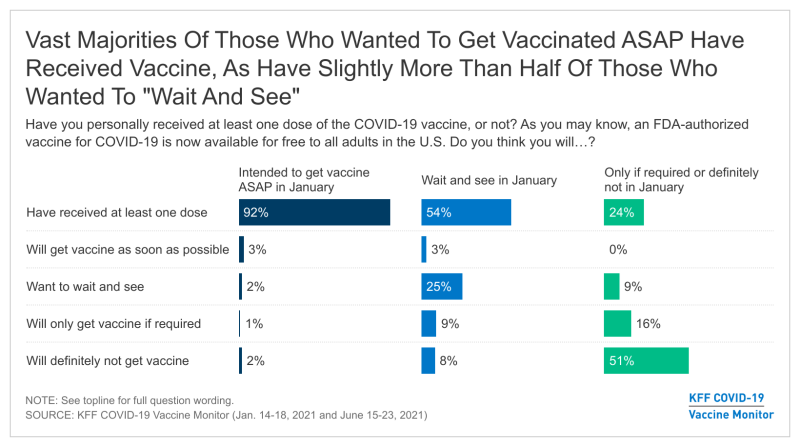
Half initially told KFF that they planned on getting vaccinated as soon as possible or had already received at least one dose. Now two-thirds say have been vaccinated, including the vast majority (92%) of those who had planned to get vaccinated “as soon as possible” in January, along with slightly more than half (54%) of those who wanted to “wait and see.” At the same time, three quarters (76%) of those who previously said they would get vaccinated “only if required” or would “definitely not” get a COVID-19 vaccine remain unvaccinated.
Importantly, one in five (21%) of all adults are now vaccinated after expressing some level of hesitation in January, saying then that they planned on waiting to get vaccinated, would only get it if required, or would definitely not get vaccinated. Many in this group cite friends, family members, and their personal doctors as influencing their decision to get a vaccine. This includes seeing friends and family members get vaccinated without serious side effects (25%), pressure from friends and family (8%), being able to safely visit family members (3%), and conversations with their personal doctors (11%). Another one in ten (9%) say that easing of restrictions for vaccinated people was a factor.
In fact, some vaccinated adults cite protecting or being able to see their friends and family members as the main reason why they decided to get vaccinated. And two-thirds (65%) say they have personally tried to persuade friends and family members to get a shot.
One-third of all adults remain unvaccinated, including 16% of adults who had previously said they planned on getting vaccinated “as soon as possible” or wanted to “wait and see” see before getting a vaccine. When asked why they changed their minds, many cite the side effects of the vaccine as a key reason.
Available through the Monitor’s online dashboard, the new report also quotes the open-ended responses given by many of those surveyed reflecting the diversity of their views and experiences related to their views and decision around vaccination.
The KFF COVID-19 Vaccine Monitor is an ongoing research project tracking the public’s attitudes and experiences with COVID-19 vaccinations. Using a combination of surveys and qualitative research, this project tracks the dynamic nature of public opinion as vaccine development and distribution unfold, including vaccine confidence and hesitancy, trusted messengers and messages, as well as the public’s experiences with vaccination.
29 Physician Specialties Ranked by Annual Compensation
During the COVID-19 pandemic, primary care physicians earned an average annual compensation of $242,000 and specialists earned an average of $344,000 — a decrease of $1,000 and $2,000, respectively, compared to before the public health crisis hit.
In its Physician Compensation Report 2021, Medscape collected responses from about 18,000 U.S. physicians across more than 29 specialties.
The latest Medscape survey was conducted from Oct. 6, 2020, through Feb. 11, 2021, after the COVID-19 crisis began.
Physicians experienced several hardships during the pandemic, including temporary office closures and restrictions on elective procedures. But in an article about its latest survey, Medscape said physician salaries were overall able to stay steady at the end of 2020, because of factors such as telemedicine reimbursement, government programs, capitation and staff reductions.
The following is annual physician compensation by specialty with the percent changes from the 2020 edition of the Medscape report, which is based on data collected from Oct. 4, 2019, through Feb. 10, 2020. This report reflects only full-time salaries. Note: The list includes a tie at No. 25. Percentages are rounded.
- Plastic surgery: $526,000 (10 percent increase)
- Orthopedics: $511,000 (0 percent)
- Cardiology: $459,000 (5 percent increase)
- Urology: $427,000 (2 percent increase)
- Otolaryngology: $417,000 (9 percent decrease)
- Radiology: $413,000 (3 percent decrease)
- Gastroenterology: $406,000 (3 percent decrease)
- Oncology: $403,000 (7 percent increase)
- Dermatology: $394,000 (4 percent decrease)
- Ophthalmology: $379,000 (0 percent)
- Anesthesiology: $378,000 (5 percent decrease)
- Surgery, general: $373,000 (2 percent increase)
- Critical care: $366,000 (3 percent increase)
- Emergency medicine: $354,000 (1 percent decrease)
- Pulmonary medicine: $333,000 (3 percent decrease)
- Pathology: $316,000 (0 percent)
- OB/Gyn: $312,000 (1 percent increase)
- Nephrology: $311,000 (1 percent increase)
- Physical medicine and rehabilitation: $300,000 (3 percent decrease)
- Neurology: $290,000 (3 percent increase)
- Rheumatology: $276,000 (5 percent increase)
- Psychiatry: $275,000 (3 percent increase)
- Allergy and immunology: $274,000 (9 percent decrease)
- Internal medicine: $248,000 (1 percent decrease)
- Infectious diseases: $245,000 (0 percent)
- Diabetes and endocrinology: $245,000 (4 percent increase)
- Public health and preventive medicine: $237,000 (2 percent increase)
- Family medicine: $236,000 (0 percent)
- Pediatrics: $221,000 (5 percent decrease)
–Gooch, Becker’s Hospital Review
CMS Pitches Physician Payment Rule for 2022: 9 Things to Know from Becker’s Hospital Review
CMS released its annual proposed changes to the Physician Fee Schedule for 2022, which expands certain Medicare telehealth provisions and updates the payment rate for physician services.
Nine things to know about the proposed rule:
- Payment rate update. With the budget neutrality adjustment to account for changes in relative value units, as required by law, and expiration of the 3.75 percent payment increase provided in 2021 by the Consolidated Appropriations Act, the proposed Physician Fee Schedule conversion factor for 2022 is $33.58, down from $34.89 in 2021.
. - Telehealth provision expansion. CMS proposed allowing certain services added to the Medicare telehealth list amid the pandemic to remain until Dec. 31, 2023, to give the agency more time to determine if the services should be permanently added following the public health emergency. CMS also said it will allow all Medicare patients to access telehealth services from their homes and is proposing to allow audio-only communication technology when used for the diagnosis, evaluation or treatment of mental health disorders.
. - Appropriate Use Criteria penalty phase delay.CMS is proposing to delay the implementation of a penalty phase of the Appropriate Use Criteria program. Currently the penalty phase is set to begin Jan. 1, but CMS proposed delaying it to Jan. 1, 2023, or the Jan. 1 that follows the end of the public health emergency.
. - Quality Payment Program changes. CMS proposed to increase the Merit-based Incentive Payment System performance threshold score providers must exceed to receive bonuses under the Quality Payment Program. CMS also unveiled the first seven optional MIPS value pathways that would begin in 2023. The seven payment pathways would be emergency medicine, chronic disease management, heart disease, anesthesia, lower-extremity joint repairs, rheumatology and stroke care.
. - Physician assistant billing. Beginning Jan. 1, physician assistants would be able to bill Medicare directly for their services and reassign payment for their services. Currently, Medicare can only make a payment to the employer or independent contractor of a PA.
. - Medicare Shared Savings program updates.CMS is proposing to give ACOs more time to transition to electronic reporting. In particular, CMS would allow ACOs to continue to use the web interface reporting option in 2022 and 2023 and phase in the new electronic clinical quality measure reporting requirement over three years. It was initially set to start in 2022.
. - Medicare Diabetes Prevention Program changes.CMS plans to waive the provider enrollment application fee for all organizations when they seek to enroll in Medicare as a Medicare Diabetes Prevention Program supplier on or after Jan. 1. CMS also proposed to shorten the prevention program services period to one year by removing the ongoing maintenance sessions phase. CMS also proposed redistributing a portion of the ongoing maintenance sessions phase payments to other core performance categories.
. - Comment solicitation.CMS is seeking provider input on two issues related to COVID-19. First, CMS wants input on what qualifies as the “home” in its preliminary policy to pay $35 add-on for certain beneficiaries when they receive a COVID-19 vaccine at home. Second, CMS is seeking comments on whether COVID-19 monoclonal antibody products should be treated the same way as other physician-administered drugs and biologics under Medicare Part B.9. Comment period. Comments on the proposed rule are due Sept. 13.
Access the full rule here.
–Paavola, Becker’s Hospital Review
Classified Ads Available for:
Physicians’ search services • allied medical placements • locum tenens • practice valuation • practice brokerage • practice consulting • real estate
For help, information or to place your ad, call Roseann Raia at 516-488-6100 ext. 302
For the MSSNY 2021 Ad Rate Sheet, please click here.
Large, fully equipped space available for lease up to 7 days per week. Includes onsite parking and is close to mass transit. Call 516-972-2986 for info.
Opportunity available at an established rheumatology practice in Great Neck, NY. Looking for a dedicated physician to join, share or merge practices. Fully equipped office with onsite parking and proximity to mass transit. Contact 516-972-2986 for more info.
Health Research, Inc. (HRI) has a job opening within the AIDS Institute’s Office of the Medical Director for a Public Health Physician II. Please distribute this announcement widely through your networks. Interested individuals can apply for this position through the HRI website.
 Small Group and Independent Practitioners – Advancing Private Practices
Small Group and Independent Practitioners – Advancing Private PracticesThe Best billing company GUARANTEED! Increase your annual revenue by 20-30%. Proven results and backed by 25 years of experience. Chooses MA MEDICLAIMS you will Save time on those RVUs/the 8-minute rule and have more time for your patient’s health. Get your free Practice analysis at www.ma-mediclaimsllc.com. Contact leslie.swartz@ma1mediclaimsllc.com or call 877-927-1996.
Office Rental 30 Central Park South
Two fully equipped exam, two certified operating, bathrooms and consultation room. Shared secretarial and waiting rooms. Elegantly decorated, central a/c, hardwood floors. Next to Park Lane and Plaza hotels. $1250 for four days a month. Available full or part-time. 212.371.0468 / drdese@gmail.com.
Medical Office and Medical Practice (Upper East Side)
79th St near Lexington / Park. 750 sq Ft beautiful, street entrance, medical office for sale with a 25 + yr internal medical practice for sale. Office is in move in condition. Physician retiring. Waiting room. Secretarial area for 3. 1 Consult room. 2 exam Rooms 2 Toilets. Please contact: 917-770-8700 / email drklein@att.net